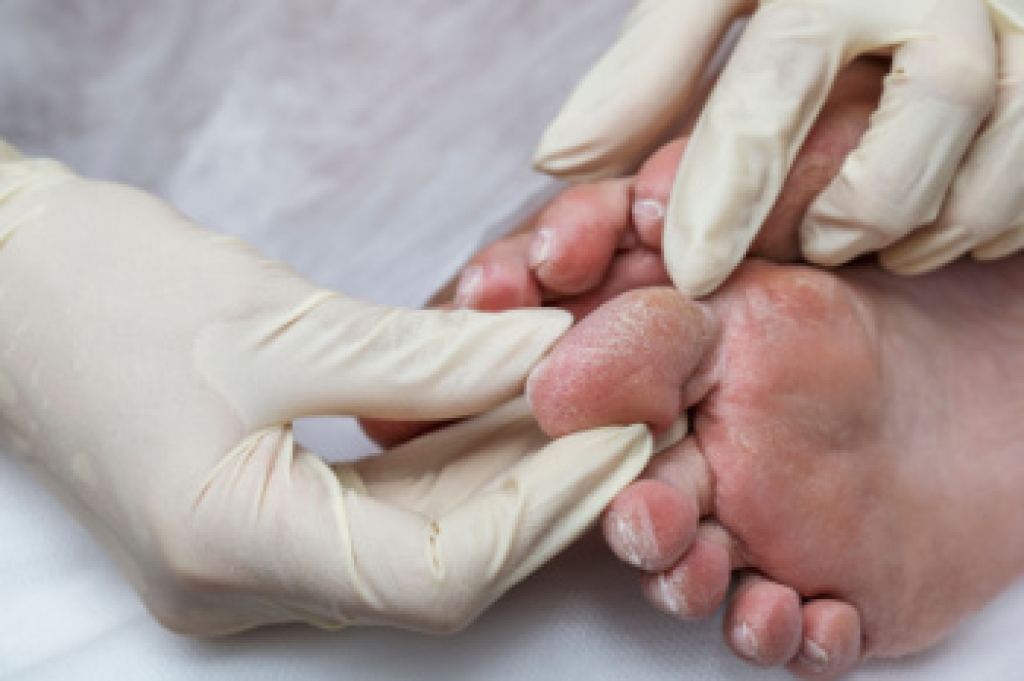
Toenail fungus and toenail mold are different infections, but both can cause changes in the appearance of the nails. Toenail fungus is caused by fungi and usually leads to thick, yellow, brittle, or crumbly nails. Toenail mold is caused by bacteria and commonly causes green, black, or dark discoloration beneath the nail. Both conditions can cause nail lifting, odor, and discomfort, but treatments are different. Risk factors include nail injuries, wearing damp shoes, and walking in moist public areas. A podiatrist can examine the nail and perform tests to identify the exact cause of the infection. Treatment depends on the type of infection and the severity of the nail damage. Early treatment is important, because untreated infections can spread to nearby skin or affect additional nails. If you have symptoms of a toenail infection, it is suggested that you schedule an appointment with a podiatrist for a diagnosis and appropriate treatment.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact Steven Black, DPM of California . Our doctor can provide the care you need to keep you pain-free and on your feet.
Symptoms
- Warped or oddly shaped nails
- Yellowish nails
- Loose/separated nail
- Buildup of bits and pieces of nail fragments under the nail
- Brittle, broken, thickened nail
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions please contact our office located in Lancaster, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.